RECOGNITION AND ASSESSMENT
Definition
- There are 2 separate presentations depending on timing of infection:
- fetal varicella syndrome (FVS): maternal chickenpox infection before 20 weeks’ gestation
- neonatal varicella (NV): maternal infection in perinatal period or close contact with chickenpox or shingles in first 7 days after birth
FETAL VARICELLA SYNDROME
Symptoms and signs
- Limb hypoplasia
- Scarring of skin in a dermatomal distribution
- Cortical atrophy, microcephaly, bowel and bladder sphincter dysfunction, vocal cord paralysis
- Chorioretinitis, cataracts and microphthalmia
- Intra-uterine growth restriction
Investigations
Maternal
- If no history of chickenpox, check maternal varicella zoster (VZ) IgG at time of contact
- If mother develops chickenpox rash, send swab from base of vesicle in viral transport media for varicella zoster PCR
Neonatal
- ≤7 days VZ IgM (can be done on cord blood), or
- >7 days VZ IgG (even if VZ IgM negative at birth)
- If vesicles present send swab from base of vesicle in viral transport media for varicella zoster PCR
Management
- Management is supportive and requires long-term multidisciplinary follow-up
- Neither varicella zoster immunoglobulin (VZIG) nor aciclovir has any role in the management of these babies
NEONATAL VARICELLA
Baby born to mother who develops chickenpox rash (but not shingles) within 7 days before birth, or 7 days after birth
- Give VZIG 250 mg (1 vial approximately 1.7 mL) IM (not IV)
- antenatal chickenpox: give as soon as possible after delivery (must be within 72 hr)
- postnatal chickenpox: give as soon as possible and within 10 days after initial exposure
- consider giving in different sites in small babies
- can be given without antibody testing of baby
- of no benefit once neonatal chickenpox has developed
- not needed for babies born after 7 days of appearance of maternal chickenpox, or where mother has zoster; these babies should have transplacental antibodies
- may not prevent NV, but can make the illness milder
- If VZIG not available or IM injection contraindicated, give 0.2 g/kg IVIG (less effective)
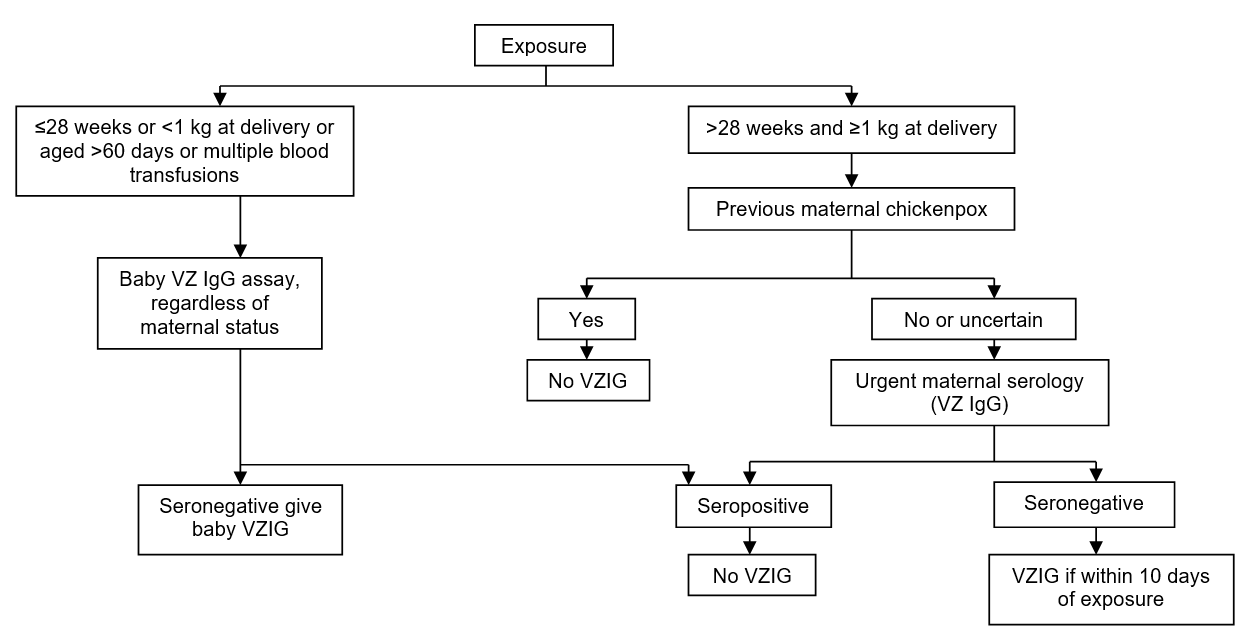
Baby exposed to chickenpox or shingles (other than in the mother)(see Decision pathway for VZV contact)
- Significant exposure: household, face-to-face for 5 min, in same room for >15 min. Case of chickenpox or disseminated shingles is infectious from 48 hr before onset of rash until crusting of lesions or day of onset of rash until crusting for those exposed to localised shingles
- Give VZIG in the following cases of postnatal exposure to varicella:
- VZ IgG-negative babies (determined by testing mother for varicella antibodies) exposed to chickenpox or shingles from any other contact other than mother, in first 7 days of life (see Decision pathway for VZV contact)
- VZ IgG-negative babies of any age, exposed to chickenpox or herpes zoster while still requiring intensive or prolonged special care nursing
- for babies exposed postnatally, regardless of maternal chickenpox history, who:
- weighed <1 kg at birth, or
- were ≤28 weeks’ gestation at birth, or
- are aged >60 days, or
- have had repeated blood sampling with replacement by packed cell infusions. Perform VZ IgG assay and, if negative, give VZIG (at risk of not having received/retained sufficient maternal VZ IgG)
Decision pathway for non-maternal VZV contact
Symptoms and signs of neonatal varicella
- Mild: vesicular rash
- Severe: pneumonitis, pulmonary necrosis, fulminant hepatitis
- mortality 30% without VZIG
TREATMENT
Aciclovir
Indications
- Babies with signs and symptoms of chickenpox aged <1 month
- If high risk (e.g. premature) and mother develops chickenpox 4 days before to 2 days after delivery
- Chickenpox in baby:
- currently treated with corticosteroids
- born prematurely
- immunocompromised
Dosage
- 20 mg/kg IV (over 1 hr) 8-hrly, diluted to 5 mg/mL
- For renal impairment, refer to Neonatal Formulary
- Treat for ≥7 days; up to 21 days if severe
SUBSEQUENT MANAGEMENT
Where
- On postnatal ward, unless baby requires neonatal intensive care support:
isolate mother and baby together in separate room until 5 days after onset of rash and all lesions crusted over
if baby already exposed, breastfeeding can continue, but explain to mother possible risk of transmission
Staff
- Exposed staff with no history of chickenpox, VZ vaccination or of unknown VZ IgG status to have VZ IgG measured by occupational health
if VZ IgG negative, immunise with varicella vaccine
remove from clinical duties during days 7–21 following exposure
if in high-risk group for complications (immunocompromised), offer VZIG
MONITORING TREATMENT
- Aciclovir
- ensure good hydration
- stop once clinical improvement occurs, or when all lesions crusted
DISCHARGE AND FOLLOW-UP
Maternal infection
- After baby has had VZIG, discharge
- Advise mother to seek medical help if baby develops chickenpox, preferably via an open-access policy where available
- Advise GP and midwife to recommend admission to isolation cubicle if rash develops
Fetal infection
- Diagnosed with positive VZ IgM or positive VZV PCR
- ophthalmic examination
- cranial ultrasound
- developmental follow-up
Date updated: