TYPES OF STOMA
Split stoma and mucus fistula
- Bowel is divided and both ends brought out through abdominal wall separately
- Proximal end is the functioning stoma and distal end is the mucus fistula
- Operation note should make it clear where the stoma and mucus fistula are situated on the abdomen
- Stoma and mucus fistula may sometimes be fashioned side-by-side without a skin bridge. The wound is closed with dissolvable sutures
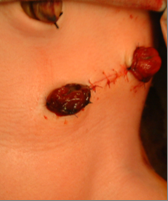
Fig.1: Split stoma and mucus fistula
End stoma without mucus fistula
- Proximal bowel end is brought out through abdominal wall as stoma and distal end is closed and left within the abdominal cavity
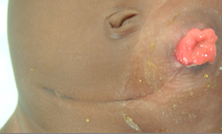
Fig. 2: End stoma without mucus fistula
Loop stoma
- Formed by suturing a loop of bowel to the abdominal wall and making an opening into bowel, which remains in continuity
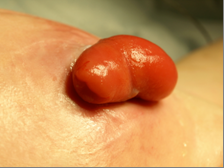
Fig 3: Loop stoma (slightly prolapsed)
MANAGEMENT
Application of stoma bag
- Before stoma starts working, fit an appropriately sized stoma bag and empty 4–6 hrly
- In a split stoma and mucus fistula, fit the stoma bag on the proximal stoma only, where possible, and leave mucus fistula exposed and dressed with a paraffin gauze dressing (e.g. Jelonet) or Vaseline® and non-sterile gauze dressing
- Change bag every 1–3 days (maximum) or if it leaks
- Remove using a stoma adhesive remover wipe
- Clean skin around stoma with warm tap water and dry with non-sterile gauze
Monitoring
- Examine baby’s abdomen and stoma daily
- Look for:
- dehydration
- abdominal distension
- wound infection or breakdown
- peri-stomal skin excoriation
- granulation tissue formation
- stomal bleeding
- discolouration of stoma or mucus fistula
- stomal prolapse or retraction
- stoma bag leakage
- rectal discharge
- If stoma becomes dusky or black, call the surgical team
- If skin surrounding the stoma is excoriated, identify cause and treat
Weight
- Babies with small bowel stoma: measure and record weight daily. Inadequate weight gain or weight loss may be secondary to:
- insufficient calorie intake
- malabsorption
- dehydration (high stoma output)
- electrolyte abnormalities (high stoma output)
Stoma effluent
- Maintain a regularly updated fluid balance chart and record:
- fluid intake and stoma losses
- colour and consistency of stoma effluent
Serum electrolytes
- Measure at least every 2 days in the first 7 post-operative days
Urinary electrolytes (sodium and potassium)
- Monitoring is extremely important for nutrition and growth
- Measure weekly
- Babies with stomata (especially small bowel stomata) are at risk of losing a significant amount of sodium into the effluent. They will often fail to gain weight if total body sodium is depleted. Serum sodium is an unreliable indicator of total body sodium
- Urinary sodium and Na+:K+ ratio are better indicators
- Sodium supplements usually required in babies with a small bowel stoma until the stoma closed
- If urinary sodium is <20 mmol/L or ratio of concentration of urinary sodium to potassium is <3:1, increase sodium intake
NUTRITION
Total parenteral nutrition and no enteral feeds
- Check surgical discharge letter and operation notes for instructions on starting enteral feeds
- Introduce enteral feeds slowly and increase gradually (see Nutrition and enteral feeding guideline)
- Useful indicators of potential feed intolerance are:
- vomiting and abdominal distension
- bile in nasogastric aspirates
- large nasogastric losses
- low stoma losses – indicating dysmotility/obstruction
- high stoma losses – indicating malabsorption
- reducing substances or fat globules in the stool/stoma effluent
Combination of parenteral nutrition and enteral feeds
- Increase enteral feeds gradually (see Nutrition and enteral feeding guideline)
- It is not possible to predict how much enteral feed baby will be able to tolerate. As a general rule, the more distal the stoma, the better the absorption of feeds
- The amount of stoma effluent and presence/absence of reducing substances or fat in the stoma effluent should guide the advancement of enteral feeds
- Do not automatically increase enteral feed in response to weight gain, but rather in response to stoma output volume
Full enteral feeds
- Tolerance of enteral feeds can fluctuate with time and babies with stomata are at high risk of life-threatening dehydration and electrolyte abnormalities as a result of gastroenteritis. There should be a low threshold for readmission to hospital and appropriate resuscitation
COMPLICATIONS
High stoma output
- Daily output >20 mL/kg/day in premature or low-birth-weight babies and 30 mL/kg/day in term babies
Measure serum and urinary electrolytes - Replace stoma losses (when >20 mL/kg/day) mL-for-mL using sodium chloride 0.9% with potassium chloride 10 mmol in 500 mL IV
- Consider either reducing or stopping enteral feeds until losses decrease, liaison with surgical team is encouraged
- Test stoma effluent for reducing substances and fat globules
- If reducing substances are positive or fat globules present, consider reduction of enteral feed or changing type of enteral feed after consultation with a surgeon, specialist surgical outreach nurse or dietitian
- Perform blood gas; (stoma effluent may be rich in bicarbonate and metabolic acidosis may be present; consider sodium bicarbonate supplementation)
Mucus fistula
- If present, consider recycling of stoma effluent (see Recycling stoma losses via a mucus fistula guideline). Before recycling, consult surgical team to decide whether a contrast study through the mucus fistula is required
- If contrast study advised, make arrangements with surgical unit and inform surgical team when the study will take place
- Surgical team will review and advise if recycling may start
- If baby not thriving, consider parenteral nutrition (see Parenteral nutrition guideline)
Increasing enteral feeds in a baby with poor weight gain and a high output stoma will worsen the situation
- If none of the above measures are effective, stop enteral feeds, start parenteral nutrition and consult surgical team to discuss surgical options
Stomal stenosis
- May be present if:
- stomal output reduces or stoma stops functioning
- stoma effluent becomes watery
- Call surgical team for advice
Prolapse
- Call surgical team for advice. If stoma is discoloured, emergency action required
STOMA CLOSURE
- Often aimed to be performed when baby is well and thriving, which may be after discharge from hospital
- Indications for early closure are:
- failure to achieve full enteral feeds
- recurrent stomal prolapse with/without stomal discolouration
- stomal stenosis
- high stoma output not responding to measures outlined above
DISCHARGE PLANNING AND PARENTAL TEACHING
- Discharge when baby well, tolerating feeds and thriving
- It is the responsibility of the ward/unit nurse to teach parents stoma care
- When discharge planned, inform:
- secretary of surgical consultant who fashioned the stoma to arrange outpatient follow-up
- local stoma care specialist to order stoma supplies for home and support family
- neonatal surgical outreach service (if involved in care)
Who to call when you need help?
Surgical team
- Call team of consultant surgeon who performed the surgery
- In an emergency out-of-hours, contact on-call surgical registrar
- Stoma care specialist [e.g. Gail Fitzpatrick at BCH (mobile 07557 001653)] for management of stoma-related complications, and parent and staff training
- Neonatal surgical outreach service [e.g. Louise Lawrence (mobile 07769 367483)] for advice, support and training on surgical management
USEFUL INFORMATION
Date updated: