DEFINITION
Congenital defect of the anterior abdominal wall resulting in herniation of bowel. The herniated viscera are not covered by any surrounding membranes and are exposed to amniotic fluid during pregnancy and air following delivery
DIAGNOSIS
- Majority of cases diagnosed on antenatal ultrasound scan
- Refer mother to fetal medicine department
- Refer parents to paediatric surgery for antenatal counselling
- Give parents gastroschisis information leaflet. Offer opportunity to visit NICU where baby will be admitted following delivery
PRE-DELIVERY
- Gastroschisis is a surgical emergency, delivery should be planned in a hospital with an appropriate level NNU aiming to transfer to paediatric surgical unit within 4 hr of birth
- Antenatal and postnatal care must be carefully planned. Communication between groups of professionals and the parents is essential
- Before delivery case to be discussed with local paediatric surgery unit
- If no surgical cot is available there and delivery cannot be postponed, then neonatal team will need to identify potential cot at nearest alternative paediatric surgical centre
- As soon as baby delivered, inform transport team
DELIVERY
- Neonatal middle grade and junior grade or ANNP attend delivery
- Take a size 8 Fr nasogastric tube (NGT) and a gastroschisis bag (often labelled as a bowel bag). This is a large sterile bag which can be closed around baby’s chest with a draw-string
- Babies become cold very quickly and experience fluid loss from the exposed bowel. Perform the following as rapidly as possible:
- clamp cord with plastic clamp (not artery forceps) placed approximately 5 cm from baby’s abdomen, checking cord clamp is securely fastened. If in doubt, apply second plastic cord clamp adjacent to the first
- dry upper part of baby quickly
- initiate resuscitation as required. Avoid prolonged mask ventilation, if resuscitation prolonged, intubate
- pass NGT (see Nasogastric tube insertion guideline) and fix securely
- empty baby’s stomach by aspirating NGT with a 10 or 20 mL syringe. If <20 mL of fluid aspirated, check position of tube
- place tube on free drainage by connecting to a bile bag
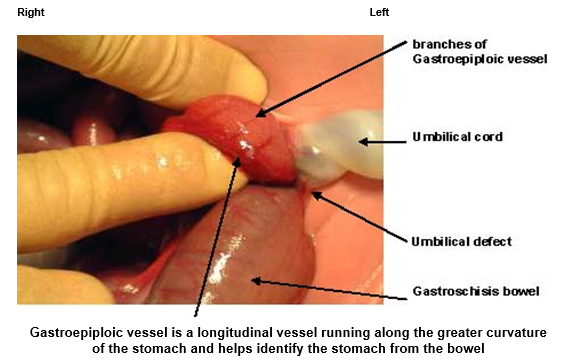
- If stomach protruding through defect (Image 1), ensure it is decompressed
Image 1
- If stomach cannot be decompressed, call surgical registrar for further advice. Failure to decompress the stomach can cause pressure on the bowel mesentery resulting in bowel ischaemia
- Aspirate NGT gently. If stomach fails to decompress, gently manipulate to facilitate this, whilst aspirating the NGT
- Take great care not to cause reflux of stomach contents up the oesophagus around the tube but simply aid drainage
- Assess colour and alignment of bowel
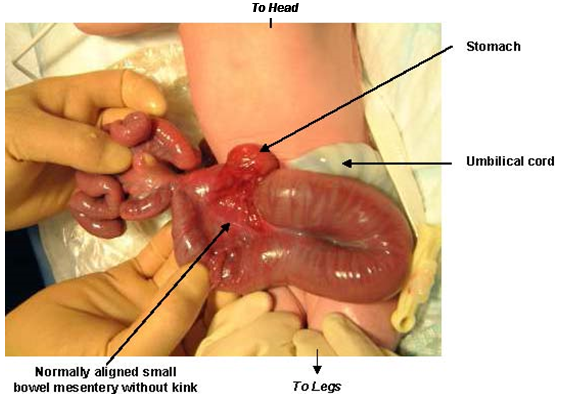
- Using sterile gloves handle the bowel carefully to ensure it is not twisted or kinked and there is no traction on the mesentery (Image 2)
Image 2
- Place baby onto the same side as the defect (usually right) and support bowel on a folded nappy placed slightly under baby
- Check perfusion of bowel. If vascular compromise suspected, contact on-call neonatal consultant
- if compromise persists, inform surgical team immediately
- Place baby’s legs and trunk into gastroschisis bag, feet first, and pull draw-string under baby’s arms, so both arms are outside of the bag
- Alternatively, cover and support intestines with cling film from upper chest to lower abdomen, holding intestines in central position
- ensure intestines are visible
- do not wrap cling film tightly as this will reduce perfusion
- Show baby to parents and transfer to NNU
- Check global perfusion using central capillary refill time (CRT)
- Check perfusion of bowel again immediately before transfer to NNU and at least every 15 min thereafter
IN NNU
- Inform transport co-ordination team immediately as this is a time critical transfer (aim to transfer to paediatric surgical unit within 4 hr of birth)
- if baby ventilated and transferring to BCH, call KIDS NTS (see Transport and retrieval guideline) (will conference call paediatric intensive care unit to arrange bed)
- if baby ventilated and transferring to a unit other than BCH, call KIDS NTS (see Transport and retrieval guideline) once PICU bed in referral hospital confirmed
- Monitor perfusion and alignment of bowel at least every 15 min
- Insert IV cannula, avoid potential long line veins
- Avoid umbilical lines
- Infuse either sodium chloride 0.9% or human albumin solution (HAS) 4.5% 20 mL/kg over 1 hr and start routine IV maintenance fluids (see Intravenous fluid therapy guideline)
- Aspirate NGT again and record volume. Replace NG losses mL-for-mL with sodium chloride 0.9% + 10 mmol potassium chloride/500 mL IV
- Monitor central perfusion, using central CRT at least every 15 min. Give further fluid boluses as required to maintain a normal CRT <2 secs. Babies with gastroschisis have a high fluid requirement until the herniated bowel is replaced in the abdomen
- Start IV antibiotics (benzyl penicillin, gentamicin and metronidazole) – see Neonatal Formulary
- Give vitamin K IM (see Vitamin K guideline)
- Discuss baby's condition and treatment plan with parents and ensure they have seen baby before transfer. Take photographs for parents
- Inform staff at surgical unit baby is ready for transfer. Have available:
- name
- gestational age
- weight
- ventilatory and oxygen requirements
- mother’s name and ward (if mother admitted), including contact number if possible (for consent)
Blood samples
Baby
- Blood culture
- FBC and clotting studies, including fibrinogen
- U&E
- Blood glucose
- Capillary/venous blood gas
- Check with surgical unit if sample from baby for group and save, Coombs or crossmatch required (e.g. Birmingham Children’s Hospital do not need these before transfer as these are done at surgical unit)
- Send 1 bloodspot on neonatal screening card marked as 'pre-transfusion' (for sickle cell screening) with baby to surgical unit
Mother
- Obtain sample of mother’s blood for crossmatch
- sample tube must be clearly hand written and labelled with mother’s name, date of birth, NHS number, and date and time of collection
- complete form
- add baby’s details to ensure it is clear sample relates to mother of baby being transferred (this information is required by surgical unit blood bank)
AWAITING TRANSFER TO SURGICAL UNIT
- Continue to assess bowel perfusion and alignment every 15 min
- Reassess baby’s fluid requirements hourly. If fluid boluses required, give sodium chloride 0.9% 10 mL/kg IV
- If evidence of a coagulopathy, treat with fresh frozen plasma (FFP) or cryoprecipitate, as appropriate (see Coagulopathy guideline)
- Aspirate NGT hourly and replace aspirate volume, mL-for-mL with sodium chloride 0.9% with 10 mmol potassium chloride/500 mL IV
- Leave NGT on free drainage
DOCUMENTATION
- Complete nursing and medical documentation for transfer. Electronically transfer any X-rays to surgical unit (or obtain copies of X-rays)
- Ensure mother’s details included (including ward phone number if an inpatient and own number if discharged) as if operation necessary and an individual with parental responsibility unable to attend surgical unit, surgeon will require verbal telephone consent
- Ensure baby’s documentation includes:
- whether vitamin K has been given
- name of referring consultant
- whether parents received antenatal counselling
- mother’s name, ward (if admitted) and her contact details
TRANSFER TO SURGICAL UNIT
- Inform surgical unit that transfer is underway
- Place baby in transport incubator, taking care to transfer bowel and mesentery in a supported, non-kinked position. Keep stomach empty
- place baby on side of defect and support bowel on a folded nappy just slightly under baby. Check bowel perfusion immediately and at least every 15 min
- ensure mother’s blood, baby’s pre-transfusion bloodspots, letters for surgical team and all documentation accompany baby
During transport
- Carry out and document usual observations, include bowel perfusion and alter its position if necessary
Arrival at surgical unit
- Record bowel perfusion and alignment
Useful information
- Parent information: https://bwc.nhs.uk/download.cfm?doc=docm93jijm4n2151
Date updated: