INTRODUCTION
- 1-5% of normal newborn babies have irregularities in heart rhythm within the first 10 days of life. These are largely self-limiting and benign
- Need to distinguish between:
- normal sinus arrhythmia (including pauses up to 1.5 sec)
- benign arrhythmias (including premature atrial and premature ventricular contractions)
- pathological arrhythmias [can be divided into tachyarrhythmias (SVT and VT) and bradyarrhythmias (congenital heart block)]
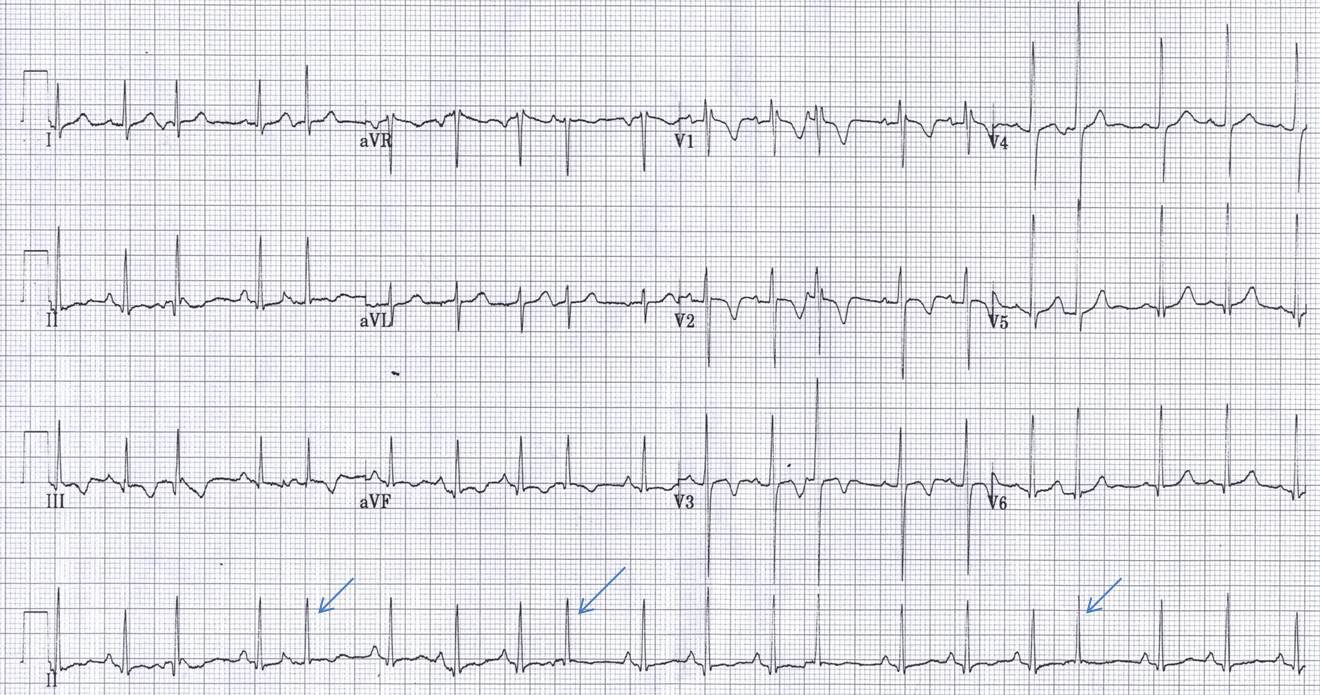
PREMATURE ATRIAL BEAT
Recognition and assessment
- Most common form of arrhythmia
- In a regular sinus rhythm at a normal rate, a P wave occurring before next expected P wave is a premature atrial beat
- Usually has a different morphology (P wave different in shape and size from normal P wave)
- Most premature atrial beats are benign
Management
- 12-lead ECG – ensure rate, rhythm and QTc are calculated
- Follow-up ECG aged 1 month (small risk of SVT)
- If premature atrial contractions persist, seek cardiology advice
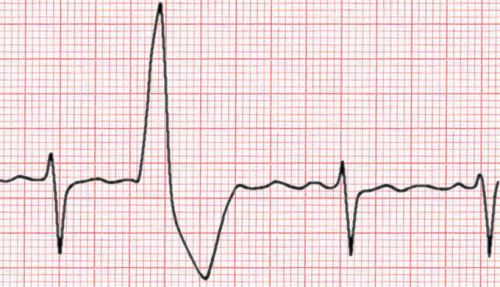
PREMATURE VENTRICULAR BEAT
Recognition and assessment
- Premature abnormal QRS complex not preceded by premature P wave
Investigations
- 12-lead ECG – ensure rate, rhythm and QTc are calculated
- Echocardiogram to rule out structural abnormality of heart
Immediate treatment
- Seek advice from paediatric cardiologist
SINUS TACHYCARDIA
Recognition and assessment
- Sinus rhythm (P wave precedes every QRS complex) with a heart rate above normal limit for age and gestation
Causes
- Fever
- Infection
- Low haemoglobin
- Pain
- Prematurity
- Hypovolaemia
- Hyperthyroidism
- Myocarditis
- Drugs (e.g. caffeine and salbutamol)
Management
- Treat the cause
- If myocarditis suspected – echocardiogram
SINUS BRADYCARDIA
Recognition and assessment
- Sinus rhythm (P wave precedes every QRS complex) with a heart rate below normal limit for age and gestation
Differential diagnosis
- Hypoxia (most likely cause)
- Vagal stimulation
- Post-intubation
- Hypovolaemia
- Hypothermia
- Metabolic derangement
- Hypopituitarism
- Obstructive jaundice
- Drugs passed from mother to baby (labetalol)
- Maternal SLE
Immediate management
- Manage airway and breathing
- If intubation required, optimise ETT position
- If bradycardia occurs post-intubation, use atropine (see Neonatal Formulary)
- Correct hypovolaemia
- Correct metabolic derangement
- If persistent, obtain 12-lead ECG
- Evaluate and treat underlying cause
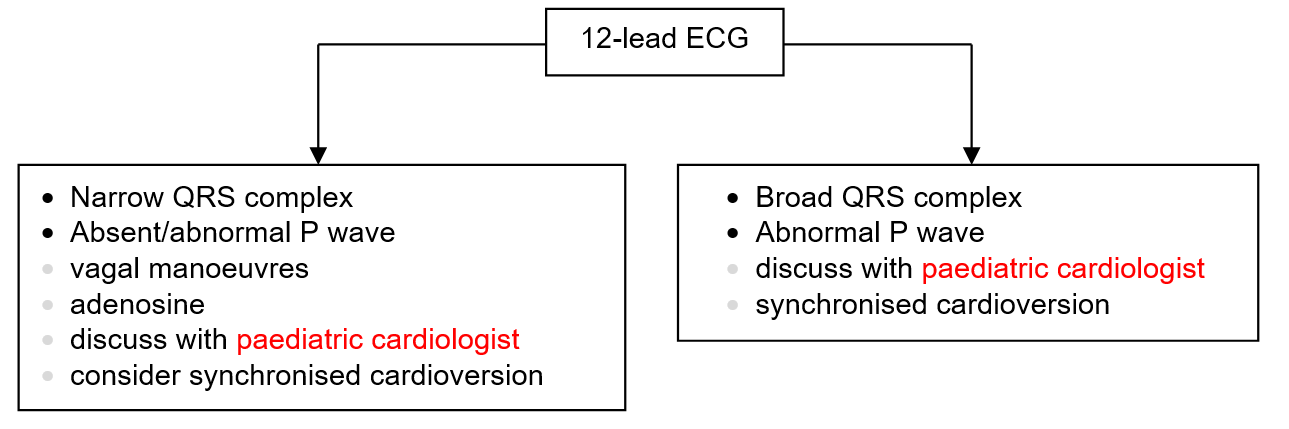
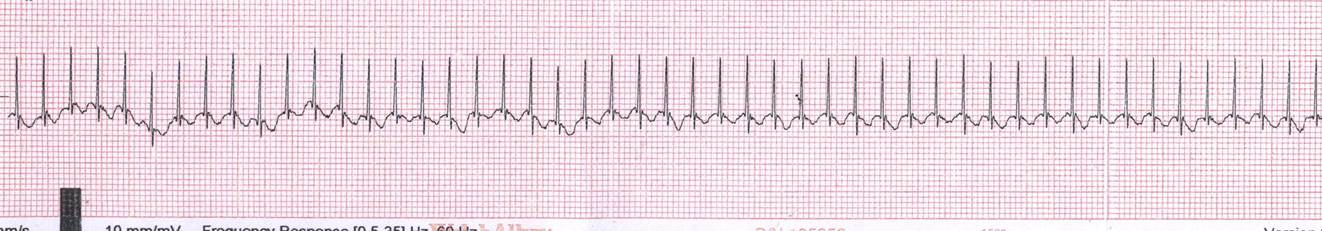
SUPRAVENTRICULAR TACHYCARDIA
Recognition and assessment
- Rapid regular tachyarrhythmia
- Heart rate >230 bpm
- ECG:
- P waves commonly absent. When present they almost always have an abnormal morphology
- narrow QRS complex
- in fast sinus tachycardia, P waves can be very difficult to see
- look for delta waves consistent with Wolff-Parkinson-White syndrome as this can affect the choice of anti-arrhythmic agent used
- For further information see Supraventricular tachycardia guideline)
VENTRICULAR TACHYCARDIA
Recognition and assessment
- Heart rate >200 bpm
- Wide QRS complexes
- ≥3 repetitive complexes
Immediate management
- Manage airway and breathing
- Correct hypoxia
- Correct electrolyte disturbance
- Discuss with paediatric cardiologist
- Consider synchronised cardioversion (in very fast heart rates, defibrillators cannot synchronise with the patient and unsynchronised will be required) if intubated, with analgesia
- Amiodarone 5 mg/kg over 30 min IV (repeat if necessary)
- If no response, lidocaine 0.5–1 mg/kg IV. May be repeated after 5 min. Maximum cumulative dose 3 mg/kg
TACHYARRHYTHMIA
- True heart rate?
- Is baby crying/in pain?
- Check airway and breathing
- Check saturation
- Consider arterial/capillary gas
- Check perfusion
- Check blood pressure
- Manage airway and breathing
- Correct hypoxia
- Correct electrolyte disturbance
Date updated: